Discover Your Best Vein Treatment Options
If you have been researching vein treatment options, you’ve most likely discovered that finding the best vein treatment for your individual condition can be quite overwhelming. Fortunately, new advances in vein treatments make them more popular, less invasive, and easier to recover from than ever. The experienced team at Vein Specialists will provide you with the latest and most effective technology for the accurate diagnosis of your vein disease and an easy-to-understand review of your vein treatment options. They will offer their best recommendations for your specific situation.
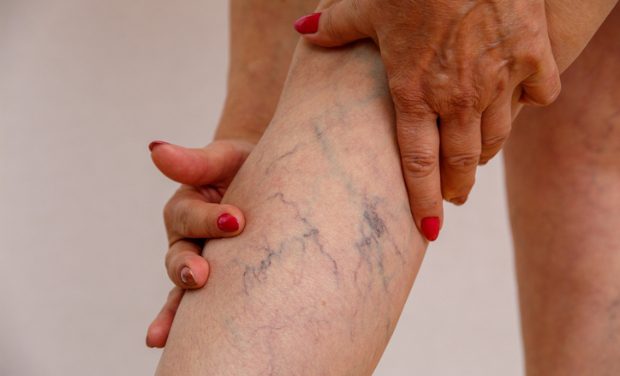
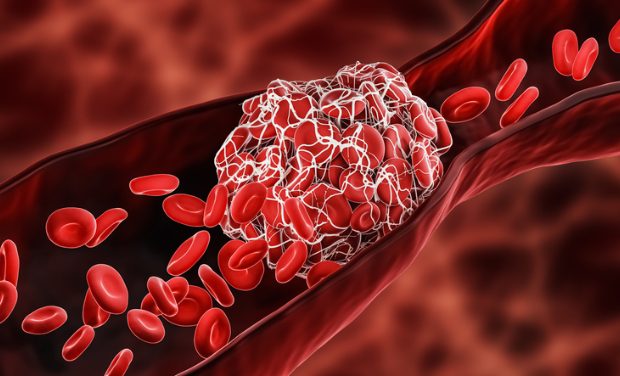
You’ve taken an important step by visiting this page. It is important to weigh the risk of leaving venous disease untreated versus obtaining a thorough evaluation, diagnosis, and successful vein treatment. The earlier you pursue a treatment option, the sooner we can help relieve and reverse your painful symptoms or signs of vein disease such as varicose veins, leg swelling, skin discoloration or leg ulcers.